When I learned I had lipedema, I cried. Hours later I was still crying. Thankfully, I was able to regain control over my thoughts, but I still struggle with depression associated with this progressive, painful and disfiguring disease.
What Is Lipedema?
Lipedema is a fat disorder. If left untreated, the disease progresses and can lead to other health problems including significant mobility issues. Even though it is estimated that nearly 11 percent of women have the disorder, lipedema is widely underdiagnosed. Lipedema almost exclusively affects women and leads to chronic physical and mental struggles. According to Dr. Karen Herbst, the leading U.S. lipedema expert, “The quality of life, emotionally and physically, for a lipedema patient often suffers because the disease is typically dismissed as simple obesity.”
leading U.S. lipedema expert, “The quality of life, emotionally and physically, for a lipedema patient often suffers because the disease is typically dismissed as simple obesity.”
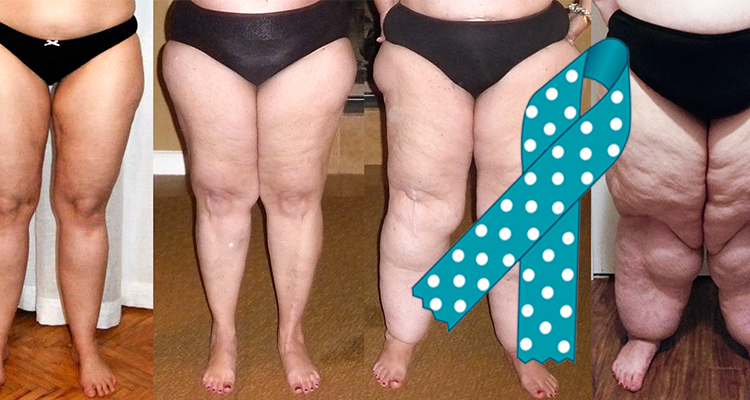
Although lipedema can be found in arms, necks, heads and elsewhere on the body, it is most commonly seen in the legs. Lipedema tissue is swollen, bumpy and feels spongy to the touch compared to non-diseased fat, which is generally soft and loose. As the disease progresses, more small marble-like structures can be felt just under the skin from where the diseased fat fuses with other tissue. Once formed, lipedema tissue cannot be dissolved through weight loss or exercise.
Pictures of me from early childhood reveal a girl of average height and weight. By age 11, however, my body began to balloon. Like most women at menarche, I gained weight in the months leading up to and after I started my first period. In fact, one year later, my weight had gone up by 70 pounds. My waist remained slender while my hips, thighs and buttocks grew larger. By the time I was 14, my lower body was out of proportion with my upper body — a classic marker of lipedema.
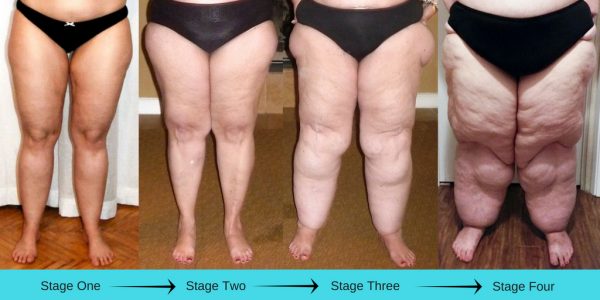
Lipedema is a progressive disease that is generally defined by four stages. The progression time from one stage to another varies widely from person to person. In fact, some sufferers do not ever move into the later stages, but determining who will progress is impossible at this point.
Lipedema was first diagnosed in the United States at the Mayo Clinic in 1940, which is ironic in a sense, given that the doctors and patients in the U.S. are widely unaware of the disease. Despite efforts by the Fat Disorders Research Society (formed in 2008) and dozens of patient advocates, lipedema is overwhelmingly misdiagnosed as obesity in this country.
The cause of lipedema is not conclusively known, but studies point to hormonal episodes (like puberty, pregnancy and menopause), genetics and stress as probable suspects. Lipedema can also appear following surgeries or other procedures that significantly disrupt hormonal systems and cause undue stress on the body.
What Is It Like to Live With Lipedema?
In early stages of lipedema, sufferers describe feeling embarrassed by their legs because of their atypical appearance including their size in relation to their upper body and texture of the skin. As the disease progresses, lipomas, or hard lumps, form along with folds of fat around the knees and down the legs that form distinct cuffs around the ankles. Lipedema patients often develop “saddlebags” of lipedema tissue on their upper thighs and hips. Obviously, many women with lipedema suffer from embarrassment and body shame, which can lead to the formation of eating disorders and other mental health challenges.
Lipedema is not only a disfiguring disease, it is also incredibly painful for most suffers. In addition to bruising easily, people with lipedema report pain upon touching the tissue and even chronic pain without contact. This pain is likely from swollen tissue, impaired lymphatic flow and chronic venous insufficiency, a corollary disease suffered by many persons with lipedema. Sufferers describe the pain from being touched or bumped as deep and burning. Something as simple as a cat jumping on the lap can send a person with lipedema into spasms of pain. The chronic pain that many sufferers feel is deep, throbbing and achy.
Eventually, as more lipedema tissue forms, sufferers can struggle with mobility. Large bulbs of lipedema fat on the inner knees can rub together while walking, which can significantly alter the gait and damage knees. In later stages of lipedema, patients can end up requiring a walker or even a wheelchair to get around.
Given the disfigurement, chronic pain and mobility issues, it is no wonder that women with lipedema report high rates of depression, anxiety and other mood disorders. Peers and adults began chastising my widening legs not long after puberty, which urged me to stop wearing shorts and swimsuits for fear of humiliation. As the disparity between my waist and hip size grew more prominent, it became harder and harder for me to find clothing that fit well. My upper body was often four or five times smaller than my lower half. Not long after, I developed binge eating disorder as a way to cope with this body embarrassment and shame, which, of course, made my physical and mental health worse.
How Is Lipedema Diagnosed?
It takes years for the average sufferer in the United States to be diagnosed with lipedema. Whether it is from fat phobic practitioners or simply ignorance about the condition, women with lipedema blame themselves for their condition. The relief that comes when the expert finally says, “This is not your fault” is muted by the horrible fact that this disease is progressive, disfiguring and does not respond to diet or exercise.
Although no blood test currently exists for diagnosing lipedema, an expertly trained physician can make the assessment through physical examination and patient history. My road to getting diagnosed was a long one. After suffering from lipedema for 32 years without even knowing it existed, Dr. John Bartholemew, a vascular specialist at the Cleveland Clinic, finally diagnosed me in October 2017.
I lived through all of those decades believing that my big legs, butt and hips were my fault. I believed that I ate too much. I was lazy. I did this to myself. Since age 11, when I first began gaining weight, I was on and off every kind of diet I could find: Richard Simmons’ Deal-a-Meal, Weight Watchers, Slim Fast, cabbage soup, low fat, low carb, and on and on and on. The results were always the same: weight loss followed by weight gain. It didn’t take long for me to develop an eating disorder, which is one of the most common side effects of chronic dieting.
Meanwhile, my lipedema areas continued to grow in both my legs and my arms, but I had no idea that my body’s resistance to weight loss was because of lipedema. Even though I had had many yearly physicals during those decades, no doctor ever mentioned lipedema to me. I realized recently that part of the reason is because none of them ever actually looked at my legs or arms.
In fact, I sought help after an online group of women suggested that I have lipedema. I had been on the keto diet — a high-fat, low-carb, moderate-protein diet — for months with no weight loss. Given these atypical results, I posted a before and after picture to a keto group, and as soon as it went live, I was inundated with messages urging me to seek help for probable lipedema. I immediately researched the condition and soon found dozens of photos of women with legs that look just like mine. Instead of feeling relieved, I felt absolutely crushed. Prior to that moment, I believed (rather falsely) that I had control over how my body felt and looked, but once I realized that the condition required extensive, expensive surgery, I lost hope and went into a dark tailspin that led me into despair.

After taking time to grieve this news, I plunged headlong into the information, found support groups online and chose a doctor. The top lipedema expert in the country, Dr. Herbst, is in Arizona and too far away to see regularly, so I chose the next best expert, Dr. Bartholomew at the Cleveland Clinic. After spending two hours examining my legs, arms, feet and abdomen, he gave me a conclusive lipedema diagnosis.
My legs and arms show all the signs of stage 2/3 lipedema:
- spongy tissue
- hard, sand-like nodules
- fat pad on the front of the knees
- fat lobes on the inner sides of the knees
- mattress-like skin texture
- pain on touch
He also told me that I have lymphedema, which is common with later stages of lipedema. It causes swelling of the extremities and pitting edema. In addition, he diagnosed me with venous insufficiency, which means that my veins have trouble circulating blood in my legs. All of these issues are responsible for the pain, tiredness and disfigurement of my legs and arms.
How Is Lipedema Treated?
Although diet and exercise will not reduce lipedema tissue, both can help reduce inflammation and other associated health issues. Eating foods that lower inflammation, like green vegetables and low-sugar fruits, can help lessen the swelling and pain, but much of what is known about dietary effects on lipedema indicates that once the tissue becomes fibrotic, no diet will successfully break it up. In fact, one of the reasons that women finally get diagnosed with the disease is because they try for years and years to diet away their excess fat with little to no results. Not all women with lipedema are obese.
The diets currently recommended by lipedema specialists for the management of inflammation include the keto diet, the rare adipose disorders diet (RAD) and low glycemic diets. Most sufferers have discovered that it takes trial and error to find an eating plan that reduces pain and swelling and can be followed long-term.
Other low-risk treatment methods include using various tools to stimulate lymphatic fluid movement. The lymphatic system runs like webs throughout the body. When the fluid collects or pools, which happens in the case of lipedema, the stagnant fluid leads to the development of enlarged fat cells that are fused to other body tissue. Therefore, keeping the lymphatic system moving is crucial to arresting or at least slowing the progression of the disease. Tools such as rebounding trampolines, vibration plates and manual lymphatic drainage (a kind of message) are effective in moving lymph fluid. Patients with lipedema also wear compression garments, use machines that press the lymphatic system and spend time in the pool, which offers both movement and compression.
In addition, several supplements have been identified as being helpful in the treatment of lipedema and its secondary diseases. According to Dr. Herbst, patients need to try different supplements and keep a log of their effectiveness. For inflammation, she recommends turmeric, fish oil and selenium. For improved lymphatic function, she recommends diosmin and butcher’s broom. The list of supplements is long and intimidating to most new lipedema patients, but with time, it becomes easier to identify which ones work best for each individual.
The gold standard in treatment for lipedema is a surgical procedure called water-assisted liposuction (WAL). It is the only known method for removing lipedema fat, eliminating pain and restoring mobility. While WAL is routinely performed in the Netherlands, Germany and other parts of Europe, it is not common in the U.S. In fact, there are a limited number of surgeons in the U.S. trained to use WAL on lipedema patients. But the leading reason many American women do not get WAL is because insurance companies refuse to pay for it, citing bans on cosmetic treatments as their reasoning. Despite multiple studies that prove that WAL removes and stops the progression of lipedema and is not a cosmetic procedure, insurance companies rarely pay for the procedure even after several appeals.
Regrettably, the out-of-pocket costs for WAL can be $50,000 or more because multiple surgeries are required to remove the tissues, and the cost almost always includes travel and accommodations. The costs are so steep in the U.S. that it is less expensive to fly to Germany, have surgery, spend weeks there recovering and fly back. It is hard to understand why insurance will not pay for WAL given that the costs of long-term pain management and mobility services will cost far more over the patient’s lifetime.
The Future of Lipedema Treatment
Knowledgeable physicians will continue to fight for insurance companies to pay for WAL surgery, and women with lipedema will continue to serve as powerful advocates for women with adipose tissue diseases. Beyond advocacy, though, other treatments are being developed that show promise for the condition
One of the most exciting tools is Quadrivas Therapy, a type of deep tissue massage developed in Vietnam and adapted by Alyna Eekema of the Netherlands. Eekema found so much success with it in curing lipedema and other fluid disorders, like lymphedema, that Dr. Herbst began a study at the University of Arizona to test the treatment. Although the pain of the procedure forced some participants to drop out, the ones who finished the trial saw major improvements in lipedema tissue and lymphatic function.
While more studies will need to be conducted before this practice is widely accepted in the U.S. to treat lipedema, the biggest challenge is training practitioners in Quadrivas Therapy. The training takes time and money. In addition, it will likely not be covered by insurance, so patients may struggle to find the means to afford the number of sessions required to completely break up the lipedema tissue and restore normal lymphatic flow. That said, for many people with lipedema, Quadrivas Therapy presents a far better option than surgery.

As for me, I know that unless a pot of gold suddenly appears in my backyard, surgery is almost certainly not an option. I manage my lipedema by spending an hour nearly every day in the pool swimming laps or walking. I wear compression as often as I can stand it. (It is hot and difficult to pull on.) I take diosmin, multi-vitamins and selenium for improved circulation. I try to lay on my back with both legs against the wall for a half an hour a day to allow my lymph system to drain naturally. I dry brush before my showers, if I remember, and I do my best to avoid foods that seem to cause swelling and inflammation in my body.
Unfortunately, I have not found any local practitioners who are knowledgeable about lipedema, but it is possible that they are out there. The nearest lipedema specialist to Wheeling is Dr. Steven Dean at the Ohio State University Wexner Center just outside of Columbus. He has an excellent reputation for being knowledgeable about lipedema and respecting the women who come to him for treatment.
It is my hope that if you are reading this article and see yourself or someone you love in my words and pictures that you will find a practitioner who will understand the disease and give you the answers you have longed for for so long. Remember this: “If you have lipedema, it is not your fault.”